The United States is currently grappling with an “out-of-control” epidemic of sexually transmitted infections (STIs), as reported by the National Coalition of STD Directors. This warning follows the release of an annual data report on STIs by the US Centers for Disease Control and Prevention (CDC).
The frustration of public health officials is palpable from the onset of the online announcement. “Yet again,” reads the CDC website, “more than 2.5 million cases of chlamydia, gonorrhea, and syphilis were reported in the United States.”
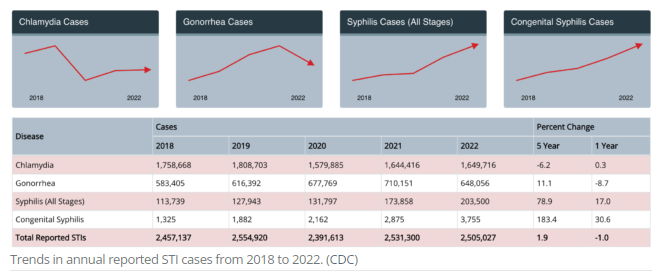
Chlamydia remains the most common STI in the US, holding its top position for years. However, it’s the recent surge in syphilis cases that is particularly alarming to health authorities.
According to CDC data, syphilis cases across all stages have surged by 80 percent in the past five years.
While the common perception revolves around adults contracting STIs, syphilis poses a threat to infants as well. When a child acquires syphilis from the mother during pregnancy or childbirth, it is termed congenital syphilis.
In 2022 alone, over 3,700 such cases were officially documented in the US, marking a staggering 937 percent increase within a decade.
The silver lining is that syphilis is treatable with appropriate antibiotics. However, the downside is that without timely diagnosis and treatment, it can inflict irreversible harm on the body. In infants, syphilis is especially perilous, sometimes leading to developmental delays, seizures, or even fatality.
In adults, syphilis spreads through vaginal, anal, or oral intercourse and typically progresses through stages. The primary stage typically involves sores around the mouth or genitals, while the secondary stage may manifest as rashes on the body and flu-like symptoms such as fever, headache, sore throat, and fatigue.
These initial stages are when the infection is most contagious. The disease rarely advances to the third stage, which can affect internal organs and be fatal.
The worrisome fact that early-stage syphilis is increasing by approximately 10 percent annually is a cause for significant concern and jeopardizes the health of infants nationwide.
Within just a year, cases of congenital syphilis have surged by 31 percent in the US, with Black or African American children disproportionately affected.
While nearly every state reported instances of congenital syphilis in 2022, Texas, California, Arizona, Florida, and Louisiana accounted for 57 percent of all cases.
Laura Bachmann, the CDC Director for STD Prevention, laments, “Tragically, these infections resulted in 282 stillbirths and infant deaths in 2022.”
Such tragic outcomes are not inevitable. Experts assert that timely syphilis testing and treatment during pregnancy could have prevented 88 percent of these cases.
So why isn’t this happening?
“The STI field has reached a tipping point,” continues Bachmann. “We’ve long recognized the prevalence of these infections, but we haven’t witnessed such severe consequences of syphilis in decades. Recent public health crises diverted program resources and exacerbated the health disparities already faced by those affected by STIs. It’s imperative that we act now to address the fallout.”
CDC officials are urging swift innovation and collaboration from all public health experts involved in STI prevention.
Their calls are echoed by numerous health associations, including the National Association of County and City Health Officials (NACCHO), the American Sexual Health Association, the American Academy of Family Physicians, and the National Coalition of STD Directors (NCSDDC).
“The CDC’s latest STI data underscores that our nation is grappling with a rapidly worsening public health crisis with real lives on the line,” states the NCSDDC.
“STIs, especially syphilis, will continue to spiral out of control unless the administration and Congress allocate the necessary funding to communities for basic screening, treatment, and prevention services.”
While President Biden has formulated a multi-agency plan to tackle America’s escalating STI cases, funding for the initiative remains uncertain.
Last year, NCSDDC Director David Harvey cautioned that if President Biden continued to slash health funding overall, his efforts toward STI prevention would inevitably falter.
“The Biden administration deserves recognition for spotlighting the most severe consequence of the nation’s STI epidemic – congenital syphilis,” notes the NCSDDC’s latest statement.
“However, we understand all too well that federal leadership will ring hollow if communities lack the funding necessary to get the job done.”